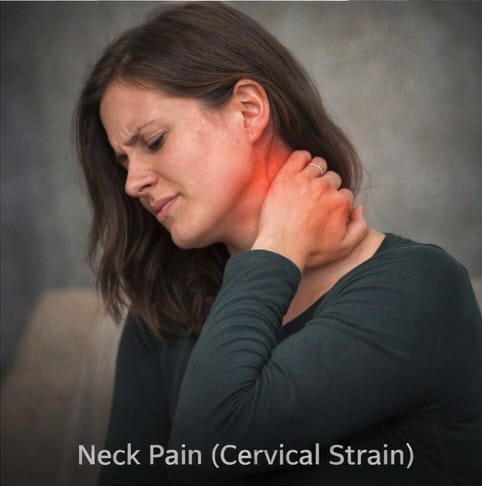
Neck pain arising from cervical strain is an extraordinarily common clinical presentation, second only to low back pain among musculoskeletal complaints driving patients to seek medical attention. The cervical spine — seven vertebrae supporting the weight of the head and allowing its complex three-dimensional movement — is particularly vulnerable to strain injuries because of the mechanical demands placed upon it throughout daily life. Poor posture during sedentary work, sudden rotational or extension forces during sport or automobile accidents, prolonged static head positions during sleep, and the cumulative effects of decades of mechanical loading all contribute to the high prevalence of cervical strain and its associated muscle pain and stiffness.
The acute phase of cervical strain, characterized by intense muscle tightness, markedly restricted range of motion, and local tenderness, significantly impairs the ability to perform basic daily activities and is often accompanied by referred pain into the shoulder, upper arm, or occiput that compounds the functional impact. Pharmacological management with centrally acting muscle relaxants — including carisoprodol — can be an important component of acute phase care, reducing the muscle spasm that is often the dominant pain driver in this period. Patients who are advised to buy carisoprodol with medical prescription for acute cervical strain management should understand its role within a comprehensive treatment strategy rather than expecting it to serve as a standalone treatment.
Anatomy of the Cervical Spine
The cervical spine’s extraordinary functional versatility — permitting flexion, extension, lateral bending, and rotation across a range of motion unmatched by any other spinal segment — comes at the cost of relative structural vulnerability compared to the more robustly supported thoracic and lumbar regions. The upper cervical segment, comprising the atlantooccipital and atlantoaxial joints, allows approximately half of total cervical rotation and a significant portion of flexion-extension. The lower cervical segment, from C3 through C7, handles the majority of flexion-extension and lateral bending, and it is here that intervertebral disc degeneration and facet joint arthrosis are most commonly found.
The muscles of the cervical region include the large superficial muscles — the trapezius, sternocleidomastoid, and splenius capitis — that provide gross movement and structural support, and the deeper intrinsic muscles — the multifidus, semispinalis, and suboccipital muscles — that provide fine motor control and segmental stability. All of these muscle groups are vulnerable to strain injuries, and virtually all develop protective spasm in response to cervical joint or disc injury. The suboccipital muscles deserve particular mention because their spasm generates headache that is referred to the occiput, vertex, and temples, frequently leading patients and clinicians to focus on the headache rather than its cervical muscular origin.
Whiplash and Cervical Strain
Whiplash-associated disorder — cervical strain produced by the rapid acceleration-deceleration forces of a rear-end motor vehicle collision — deserves particular discussion because of its prevalence and the clinical complexity of its management. The mechanism involves a biphasic injury: first a rapid extension of the lower cervical spine as the torso is driven forward while the head initially remains in place, followed immediately by rebound flexion as the head is carried forward and then restrained by the safety harness. This biphasic motion loads the anterior and posterior cervical structures in rapid succession, producing a pattern of soft tissue injury that may involve anterior disc and ligamentous structures, posterior facet joint capsules, and the paraspinal musculature.
The pain and stiffness of whiplash-associated disorder may be delayed by twelve to twenty-four hours after the injury due to the inflammatory cascade that develops progressively over this period. Patients who present initially without severe symptoms may return the following day in considerably greater discomfort, which can lead to both patient anxiety and diagnostic confusion. Early pharmacological management with analgesics and muscle relaxants — prescribed after appropriate clinical assessment to exclude fracture and neurological injury — can reduce the severity of the acute pain phase and facilitate the early mobilization that is the most important prognostic intervention in whiplash-associated disorder.
Carisoprodol in Cervical Strain Management
In the acute phase of cervical strain, muscle spasm of the paraspinal, trapezius, and sternocleidomastoid muscles is often the dominant pain source and the primary functional limitation. Carisoprodol’s central mechanism of action — reducing excessive motor output through polysynaptic spinal reflex arc disruption — directly targets this spasm-driven component of pain, making it pharmacologically well-suited to acute cervical strain management. By reducing paraspinal hypertonicity, it enables greater neck mobility, facilitates the application of physical therapy techniques that would otherwise be too painful to tolerate, and allows patients to achieve more comfortable sleeping positions that improve sleep quality and recovery.
Patients who order carisoprodol with a valid prescription from their physician for acute cervical strain should use it as directed and understand that its role is to support the natural healing process by reducing the spasm barrier to movement, not to eliminate all pain or serve as a permanent management solution. The drug’s sedating properties are particularly relevant for cervical strain patients who experience difficulty sleeping due to positional neck pain, and the bedtime dose can meaningfully improve sleep quality during the acute recovery period.
Complementary Treatment Modalities
Physical therapy is the most important non-pharmacological intervention in cervical strain management. Techniques including cervical mobilization and manipulation, trigger point release of the suboccipital and upper trapezius muscles, postural retraining, and progressive cervical strengthening exercises address the structural and muscular contributors to pain in ways that pharmacological treatment alone cannot. Heat application to the cervical musculature promotes local blood flow and facilitates muscle relaxation. Transcutaneous electrical nerve stimulation provides additional analgesic benefit through gate-control mechanisms in some patients.
Cervical collars — soft foam supports that restrict neck movement — are appropriate only for the most acute phase of severe whiplash or strain and should not be used beyond the first few days, as prolonged immobilization promotes muscle deconditioning and delays recovery. Ergonomic assessment of the patient’s workstation, sleep position, and daily head posture habits provides an essential foundation for preventing symptom recurrence. Monitor height adjustment, appropriate pillow selection, and avoidance of prolonged smartphone use in flexed neck positions are among the most impactful ergonomic modifications.
Prognosis and Prevention
The majority of acute cervical strain episodes resolve substantially within four to eight weeks with appropriate management. The pharmacological role of carisoprodol is confined to the most acutely painful initial period, and patients should not continue the medication beyond the prescribed course. Those who purchase carisoprodol at the pharmacy as part of acute cervical strain management should be aware that the goal is to bridge through the most painful phase, not to maintain indefinite pharmacological muscle relaxation.
Preventing recurrence requires addressing the postural, ergonomic, and biomechanical factors that predispose to cervical strain. Regular cervical and upper trapezius stretching exercises, attention to head and neck posture during prolonged desk work, limitation of smartphone use in forward-head postures, and appropriate cervical strengthening exercises all reduce vulnerability to future episodes. For patients with recurrent cervical strain or underlying cervical spine degeneration, periodic physiotherapy reassessment allows early identification of developing dysfunction before it progresses to a more severe and protracted episode.