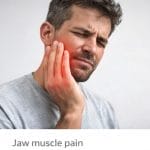
Temporomandibular joint disorder is a clinical syndrome that affects a surprisingly large proportion of the adult population — estimates consistently place prevalence between five and twelve percent in Western countries — yet it remains among the most consistently undertreated and misunderstood chronic pain conditions in outpatient medicine. The temporomandibular joint, which connects the mandible to the temporal bone of the skull on each side of the face, is one of the most mechanically active joints in the human body, required to perform thousands of opening, closing, and lateral excursion movements each day during chewing, speaking, swallowing, and yawning. When the articular mechanics of this joint become disrupted — through disc displacement, articular cartilage degeneration, ligamentous laxity, or the massively increased compressive loading produced by bruxism and chronic jaw clenching — the consequences extend far beyond the joint space itself. The surrounding masticatory muscles develop reactive spasm, myofascial trigger points, and persistent hypertonicity that constitute the primary pain source for the majority of patients with temporomandibular joint disorder and that are responsible for the temporal headache, preauricular pain, earache, and jaw stiffness that dominate the clinical presentation.
The muscle tension component of temporomandibular joint disorder responds to centrally acting muscle relaxants, and patients evaluated by a physician or oral and maxillofacial specialist who present with severe masticatory muscle spasm may be advised to buy carisoprodol with medical prescription as a short-term adjunct to reduce hypertonicity during the most acute phase of their disorder. Carisoprodol, by disrupting the polysynaptic spinal reflex arcs that sustain involuntary muscle contraction, reduces the excessive tone in the masseter, temporalis, and pterygoid muscles that is both painful in itself and a perpetuating factor for articular stress within the temporomandibular joint.
Anatomy and Mechanisms of Masticatory Muscle Spasm
The muscles of mastication are a functionally integrated group comprising four primary muscles — the masseter, temporalis, medial pterygoid, and lateral pterygoid — whose coordinated activity drives all mandibular movements. The masseter, the most superficially located of these muscles running from the zygomatic arch to the angle of the mandible, is the primary jaw-closing muscle and the one most directly affected by bruxism-related overuse. Its deep and superficial heads contain a high density of muscle spindles and proprioceptive receptors that are responsive to both mechanical strain and to the elevated sympathetic nervous system tone that accompanies psychological stress, making it exquisitely sensitive to the combination of postural and emotional factors that drive temporomandibular joint disorder in most patients.
Myofascial trigger points — discrete hypersensitive nodules within taut bands of muscle fiber that generate local tenderness and characteristic patterns of referred pain when compressed — develop within the chronically overloaded masseter and temporalis with extraordinary frequency in temporomandibular joint disorder. Trigger points in the masseter refer pain to the cheek, the angle of the jaw, the upper and lower molar teeth, and the temporal region in patterns that patients often describe as toothache or earache, leading to inappropriate dental extractions and ENT investigations before the masticatory muscle origin of the pain is recognized. Temporalis trigger points generate referred pain to the temporal region, the forehead, and across the maxillary teeth in patterns that precisely mimic tension-type headache, explaining the high co-occurrence of temporomandibular joint disorder and chronic daily headache in clinical populations.
The pathological muscle tension of temporomandibular joint disorder is not simply a passive response to articular pathology but an active, centrally mediated process that becomes self-sustaining once established. The sustained hypertonicity of the masticatory muscles produces ischemia within the contracting fibers, metabolite accumulation, and sensitization of intramuscular nociceptors that generate ongoing pain signals. These pain signals feed back into the central nervous system to reinforce the motor output maintaining muscle contraction, perpetuating the spasm-pain-spasm cycle that is the defining pathophysiological feature of the muscular subtype of temporomandibular joint disorder.
Clinical Features and Diagnosis
The clinical presentation of temporomandibular joint disorder encompasses a predictable constellation of symptoms that, when recognized as a cluster, permit confident clinical diagnosis without requiring advanced imaging in most cases. Jaw pain — typically described as a dull, aching discomfort in the preauricular region and the angle of the jaw that worsens with chewing, prolonged talking, or wide mouth opening — is the most consistently reported symptom. Morning jaw soreness, representing the accumulated muscular fatigue of nocturnal bruxism activity, is highly characteristic and clinically informative. Restricted mouth opening — a maximum interincisal distance below 40 mm in adults — reflects either masticatory muscle spasm limiting movement or articular disc pathology mechanically blocking condylar translation, and distinguishing between these causes guides appropriate treatment.
Associated headache in the temporal distribution, earache without otological pathology, tinnitus, and cervical pain are frequent co-occurring symptoms that reflect the referred pain patterns of masticatory muscle trigger points and the cervical dysfunction that commonly coexists with temporomandibular joint disorder in clinical practice. The physical examination should include measurement of maximum mouth opening and the pattern of jaw deviation during opening, bimanual palpation of the temporomandibular joints for tenderness and joint sounds, systematic muscle palpation of the masseter, temporalis, and medial pterygoid for tenderness and trigger points, and evaluation of cervical range of motion and upper cervical tenderness.
Pharmacological Management
The pharmacological management of temporomandibular joint disorder-related muscle tension targets multiple aspects of the pain-generating cascade. NSAIDs reduce the prostaglandin-mediated nociceptor sensitization within the inflamed masticatory muscles and joint tissues, providing analgesic and anti-inflammatory benefit. Low-dose tricyclic antidepressants — particularly amitriptyline at 10 to 25 mg at bedtime — address the central sensitization driving the chronification of masticatory muscle pain and additionally reduce nocturnal bruxism intensity through their effects on sleep architecture, making them particularly appropriate for patients with temporomandibular joint disorder dominated by nocturnal bruxism.
For patients with severe acute masticatory muscle spasm producing significantly restricted mouth opening, intense pain, and inability to tolerate dental treatment or physical therapy, short-term centrally acting muscle relaxants provide the most direct pharmacological relief. Those directed to order carisoprodol at the pharmacy after physician evaluation for severe temporomandibular joint disorder-related spasm should use the medication for the shortest effective duration — typically two to three weeks — combining it with dental management and physical therapy that address the structural and behavioral contributors to masticatory muscle overload. The centrally acting mechanism of carisoprodol targets the reflex hypertonicity that drives masticatory muscle spasm in ways that peripheral analgesics cannot replicate, providing a therapeutic adjunct that facilitates participation in the manual therapy and exercise-based interventions that produce the most durable improvements.
Botulinum toxin injection into the masseter and temporalis — performed by trained oral and maxillofacial surgeons or orofacial pain specialists — represents an important longer-term pharmacological option for refractory masticatory muscle spasm, reducing muscle bulk and resting tone for three to four months per treatment cycle. Multiple clinical trials support its efficacy for temporomandibular joint disorder-related pain and bruxism, and it may reduce the need for ongoing oral muscle relaxant therapy in patients who achieve good responses to injection treatment. The combination of short-term oral carisoprodol for acute symptom management alongside planning for botulinum toxin injection as longer-term maintenance represents a rational sequential pharmacological strategy for severe refractory masticatory muscle spasm.
Dental and Physical Therapy Management
Occlusal stabilization splints — custom-fabricated acrylic appliances worn over the teeth, typically during sleep — are the most widely used and evidence-supported dental intervention for temporomandibular joint disorder, reducing compressive forces on the joint and providing a physical barrier against tooth-to-tooth contact during nocturnal bruxism. They do not eliminate the central neurological drive producing bruxism but consistently reduce its mechanical consequences for the joint and masticatory muscles. Patients whose temporomandibular joint disorder is driven primarily by dental malocclusion may benefit from occlusal adjustment, orthodontic treatment, or prosthodontic rehabilitation to reduce the structural contributors to masticatory muscle overload.
Physical therapy for temporomandibular joint disorder combines manual therapy techniques — including myofascial release of the masseter and temporalis, intraoral trigger point treatment of the pterygoid muscles, and cervical mobilization for the frequently coexisting cervical dysfunction — with therapeutic exercises targeting jaw mobility, masticatory muscle coordination, and postural alignment. The combination of dental management, physical therapy, and appropriately supervised pharmacological support with agents including carisoprodol when purchased with medical prescription from a licensed physician produces superior outcomes to any single modality in isolation, addressing the multiple structural, muscular, and behavioral contributors to temporomandibular joint disorder-related pain in a comprehensive and coordinated fashion.